Translate this page into:
Dermoscopy as a Saviour in Psoriasiform Lesion
*Corresponding author: Siddharth Mani, Department of Dermatology, Sanjivani Hospital, Kochi, Kerala, India. smani5931@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Mani S. Dermoscopy as a Saviour in Psoriasiform Lesion. Indian J Postgrad Dermatol 2023;1:134-5.
Dear Sir,
COVID times have made the dermatology practice very tricky with the doctors in a constant dilemma of choosing between physical examination vis-a-vis teleconsultation. Teleconsultation although very useful has its limitations, with not being able to examine the patient physically, being the chief constraint. Apart from this, a limited number of biopsies were being done to reduce the exposure time. Herein, we present a case of an infant who had a psoriasiform lesion in the occipital area and was being managed as a case of psoriasis on teleconsultation.
An 8-month-old female infant presented with a history of scaly lesions over the scalp for the past 6 months. The lesion was painless and was associated with some scaling. The child was irritable with constant itching over the lesion. Parents informed that there was an initial erythematous lesion over which scaling had developed over the past 2 months. There was no history of similar lesions in any family members. Her mother denied any involvement of palms, soles, nails or mucosa. The patient was consulted through WhatsApp and a provisional diagnosis of childhood psoriasis was given. The patient was started on topical desonide to which she partially responded. The patient reported to the clinic physically after 2 months of taking initial treatment. At this time, there was 7 × 3 cm, irregular, erythematous, scaly plaque present over the occipital area [Figure 1]. The lesion was non-tender. A differential diagnosis of seborrheic dermatitis, nevus simplex with Meyerson phenomenon and psoriasis was considered. A grattage test was done to demonstrate the Auspitz sign, but the test came out to be negative which put the diagnosis of psoriasis in doubt. Hence a dermoscopic examination was performed which revealed the presence of irregular linear vessels [Figure 2]. Absence of diffuse yellowish scales, single and clusters of scales on an erythematous background distributed among the follicular units, peripilar casts, thin arborizing vessels, multicomponent vascular pattern – constituted by multiple dotted, comma, linear and small arborizing vessels – and simple red loops helped in ruling out seborrheic dermatitis. Parents denied biopsy of the lesion. Based on clinical and dermoscopic examination, the child was diagnosed with a case of nevus simplex with the Meyerson phenomenon.
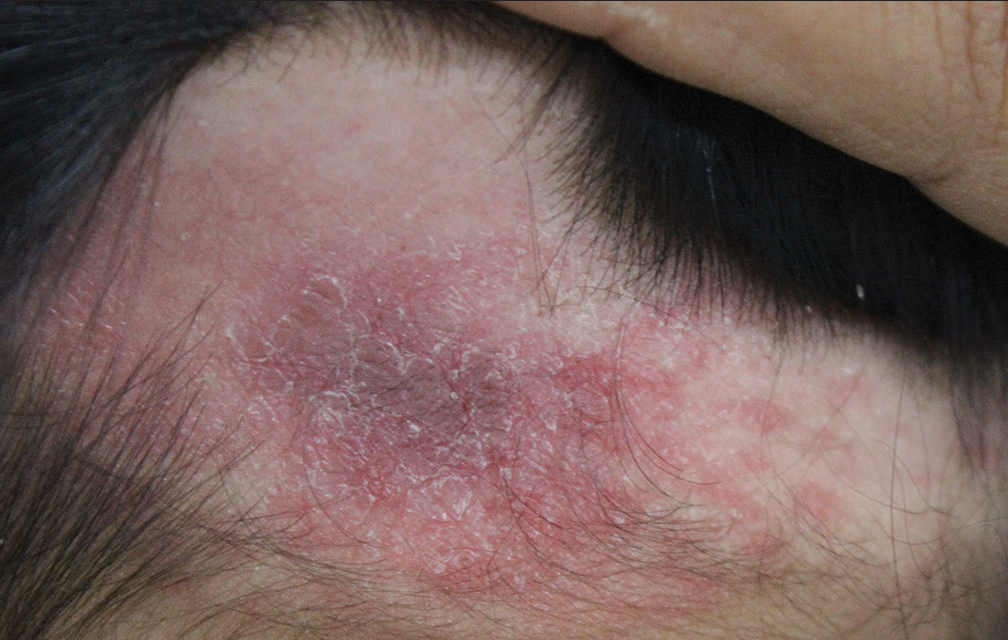
- Solitary 7 × 3 cm, irregular and erythematous scaly plaque present over the occipital area.
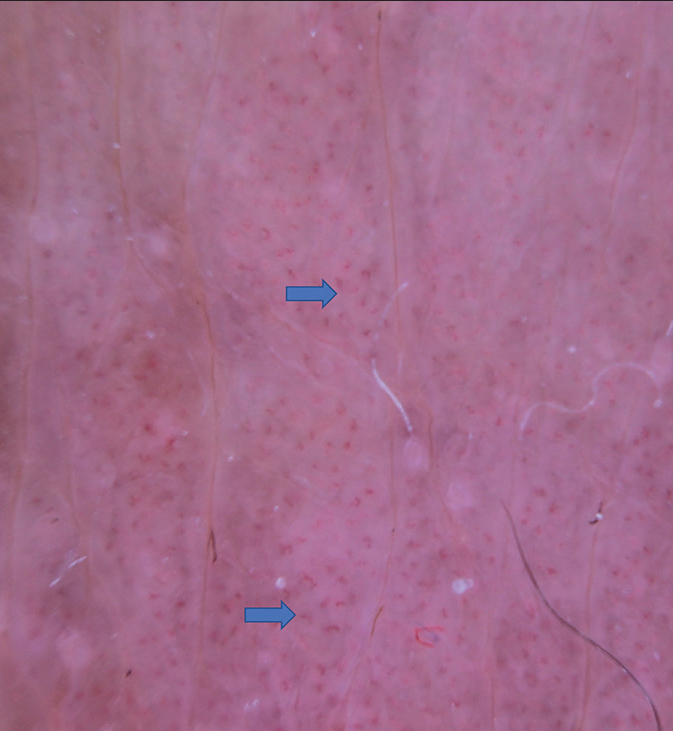
- Dermoscopy reveals the presence of irregular linear vessels (Blue arrows).
The Meyerson phenomenon, also called halo eczema or halo dermatitis, represents an eczematous reaction over a pre-existing cutaneous lesion. It leads to alteration in the morphology of the original lesion which is responsible for diagnostic difficulty. The phenomenon was initially described by Meyerson in 1971 in benign melanocytic nevi.[1] However, the term was proposed much later in 1988 by Nicholls and Mason.[2] Apart from the melanocytic lesion, other conditions where this phenomenon is positive include seborrheic keratosis, dermatofibroma, molluscum contagiosum, keloid and nevus sebaceous. Very rarely, Meyerson phenomenon has also been reported in vascular malformations such as nevus simplex, port wine stain and capillary malformation of limb and trunk.[3] Most patients with the Meyerson phenomenon associated with capillary malformation have scaling, confined to the area of malformation as was seen in our case.[4] Although the exact pathogenesis is not clear, it is stipulated that the phenomenon associated with a capillary malformation is due to vascular stasis and sensitisation to autoantigens. Aberrant expression of intercellular adhesion molecule-1 and increased number of CD4 T-cells also play an important role in its pathogenesis.[5] The presence of this phenomenon casts a diagnostic difficulty as evident from our case; hence, the role of a dermoscope in such cases which help in quick bedside/out patient department (opd) examination cannot be emphasised more. Dermoscopy of capillary malformation shows linear vessels, irregular reticular vessels, dotted vessels and globular vessels.[6] Our case showed the presence of irregular linear vessels. Even though dotted vessels have been described in the literature for capillary malformation, they are irregular as compared to regular dots of psoriasis. The patient was managed with topical steroids with which the scaling decreased. Parents were, then, counselled regarding the prognosis of nevus simplex and the possibility of using pulse dye laser later in life, in case the lesion persists.
Meyerson phenomenon overlying nevus simplex has sparingly been reported. Our case underscores the importance of the use of a dermoscope to differentiate between psoriasis and the Meyerson phenomenon overlying capillary malformation.
Declaration of patient consent
Patient’s consent not required as patients identity is not disclosed or compromised.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The author(s) confirms that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- A Peculiar Papulosquamous Eruption Involving Pigmented Nevi. Arch Dermatol. 1971;103:510-2.
- [CrossRef] [PubMed] [Google Scholar]
- Halo Dermatitis Around a Melanocytic Nevus: Meyerson's Nevus. Br J Dermatol. 1988;118:125-9.
- [CrossRef] [PubMed] [Google Scholar]
- Meyerson Phenomenon Over Nuchal Nevus Simplex. Dermatol Pract Concept. 2021;11:e2020098.
- [CrossRef] [PubMed] [Google Scholar]
- Eczema within a Capillary Malformation: A Case of Meyerson Phenomenon. Ann Dermatol. 2016;28:781-2.
- [CrossRef] [PubMed] [Google Scholar]
- Dermoscopic Features of Port-wine Stains: A Study of 264 Cases. Australas J Dermatol. 2021;62:e201-6.
- [CrossRef] [Google Scholar]
- Itchy Capillary Malformations: Unusual Appearance of Meyerson Phenomenon, a Case Series. Pediatr Rep. 2021;13:131-4.
- [CrossRef] [PubMed] [Google Scholar]






