Translate this page into:
Primary Cutaneous Aspergillosis in an HIV Patient and Combined Therapy: A Case Report
*Corresponding author: Marla Lucero Vega-Santoyo, Department of Internal Medicine, Regional General Hospital No. 1 “Dr. Carlos Mac Gregor Sánchez Navarro”, Mexico City, Mexico. marla.lvsantoyo@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Méndez-Flores S, Vega-Santoyo ML, Hernández-Hernández F. Primary Cutaneous Aspergillosis in an HIV Patient and Combined Therapy: A Case Report. Indian J Postgrad Dermatol. doi: 10.25259/IJPGD_18_2024
Abstract
Primary cutaneous aspergillosis (PCA) is a rare disease caused by a few pathogenic species of Aspergillus. It manifests in immunocompromised patients as different types of localised lesions, the treatment has evolved and the latest reviews ensure better results with a combined therapy. We present a 27-year-old male gardener with a history of human immunodeficiency virus infection and a nodular presentation of PCA. He received surgical and antifungal medication, showing a good response and no dissemination or recurrence of the disease.
Keywords
Primary cutaneous aspergillosis
Human immunodeficiency virus
Aspergillus fumigatus
Fungal infection
Itraconazole
INTRODUCTION
Primary cutaneous aspergillosis (PCA) is an invasive fungal infection where the skin serves as the primary source of the disease.[1] It is more common in individuals with immunosuppression. Associated conditions include blood malignancies, human immunodeficiency virus (HIV), solid organ transplantation and the use of steroids; among other risk factors, occupations linked to its inoculation and development are gardening and farming.[2] The clinical presentation varies, but the typical manifestation of cutaneous aspergillosis consists of a black eschar located on a red plaque, typically localised at the site of a skin injury.[3] Most often, it is associated with intravenous catheters or the occlusive dressings used for them.[4] The combination of direct microscopy, culture and histopathological examination represents the gold standard in diagnosing PCA, as well as invasive aspergillosis.[5]
Since the 1980s, cases associated with HIV have been reported, exhibiting distinct characteristics from patients without this disease. This case study aims to provide insights into the nodular presentation features in HIV patients and their outcomes. This holds significance as the identification of this disease bears the potential to progress into a systemic infection, thereby amplifying mortality rates among afflicted individuals.[4]
CASE REPORT
A 27-year-old male born and raised in Mexico City works as a gardener. He had a history of HIV infection and was treated with abacavir, lamivudine and efavirenz. His last CD4 count was 258 cells/mm3, and his viral load was 20,000 copies/mL. He had a previous Mycobacterium avium complex infection in 2009 and was treated with ethambutol, clarithromycin and prednisone (35 mg/day), with no other significant medical history. He presented to the office with a 7-month history of an asymptomatic, erythematous, 7 mm diameter nodule with superficial erosion in the centre, located on his right hand, affecting the lateral metacarpal area [Figure 1]. He denied any previous trauma. There were no significant findings on systemic examination, and other investigations, including a chest X-ray, abdominal ultrasound scan and chest computed tomography, were all unremarkable.
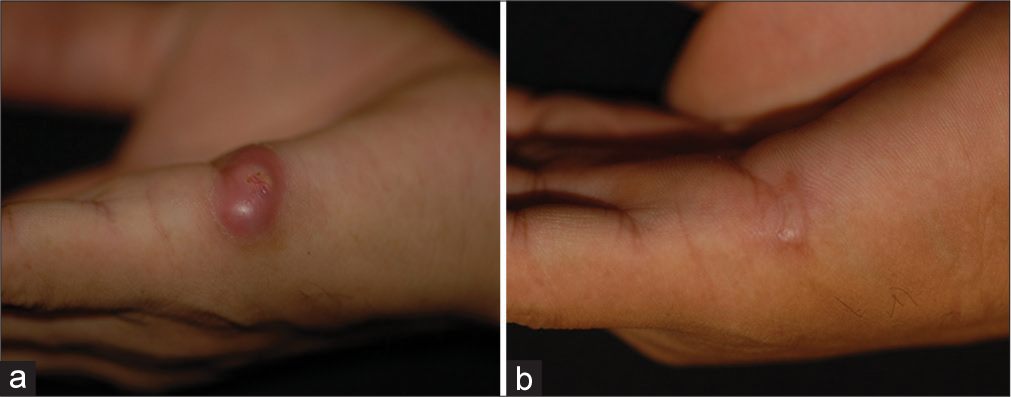
- (a) An erythematous, stiff, 7 mm diameter nodule with superficial erosion in the centre, localised to the right hand, affecting the lateral metacarpal area. (b) Resolution of the lesion after treatment.
A biopsy was performed suspecting an underlying fungal aetiology. Culture on Sabouraud medium showed velvety olive-green colonies with a whitish peripheral halo, and direct examination revealed septate, hyaline and branched mycelium. In the histological sections stained with periodic acid-Schiff (PAS), we observed multiple septate hyaline hyphae, with cross-sectional, longitudinal and oblique cuts of the same [Figure 2].
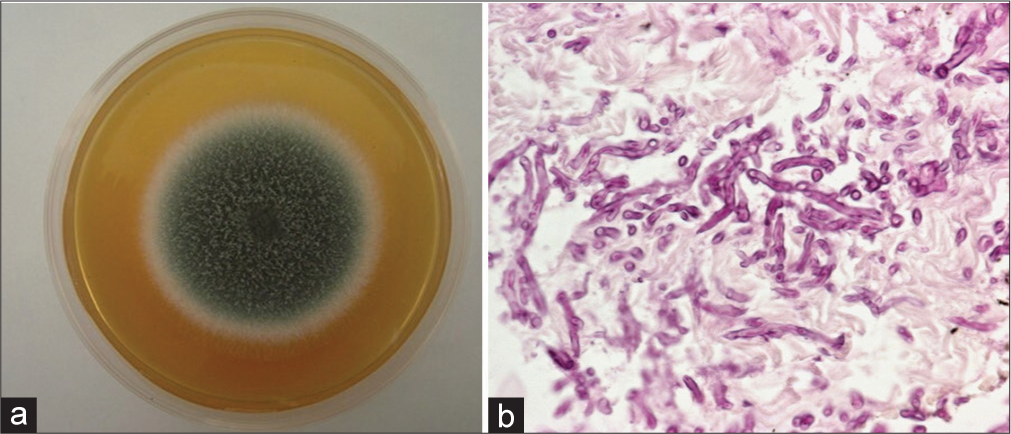
- (a) Tissue culture on Sabouraud medium: Velvety colonies with an olive-green coloration and a whitish peripheral halo (b) Histological sections stained with periodic acid-Schiff: Multiple septate hyaline hyphae, including cross-sections, longitudinal sections and oblique sections 40x.
In the direct examination of cultures under the microscope, we observed septate, tabulated and hyaline mycelium, as well as Aspergillus heads composed of long conidiophores, round vesicles from which two series of phialides emerged and round microconidia originating from the latter [Figure 3]. With these findings, PCA by Aspergillus fumigatus was diagnosed. For the patient’s treatment, surgical excision of the lesion was performed initially, followed by pharmacological treatment with a daily dose of itraconazole 200 mg for 6 months. After the treatment period, clinical resolution was documented. Subsequently, mycological resolution was confirmed by performing a punch biopsy at the site of the initial lesion, which yielded negative results, and there was no recurrence during the follow-up.
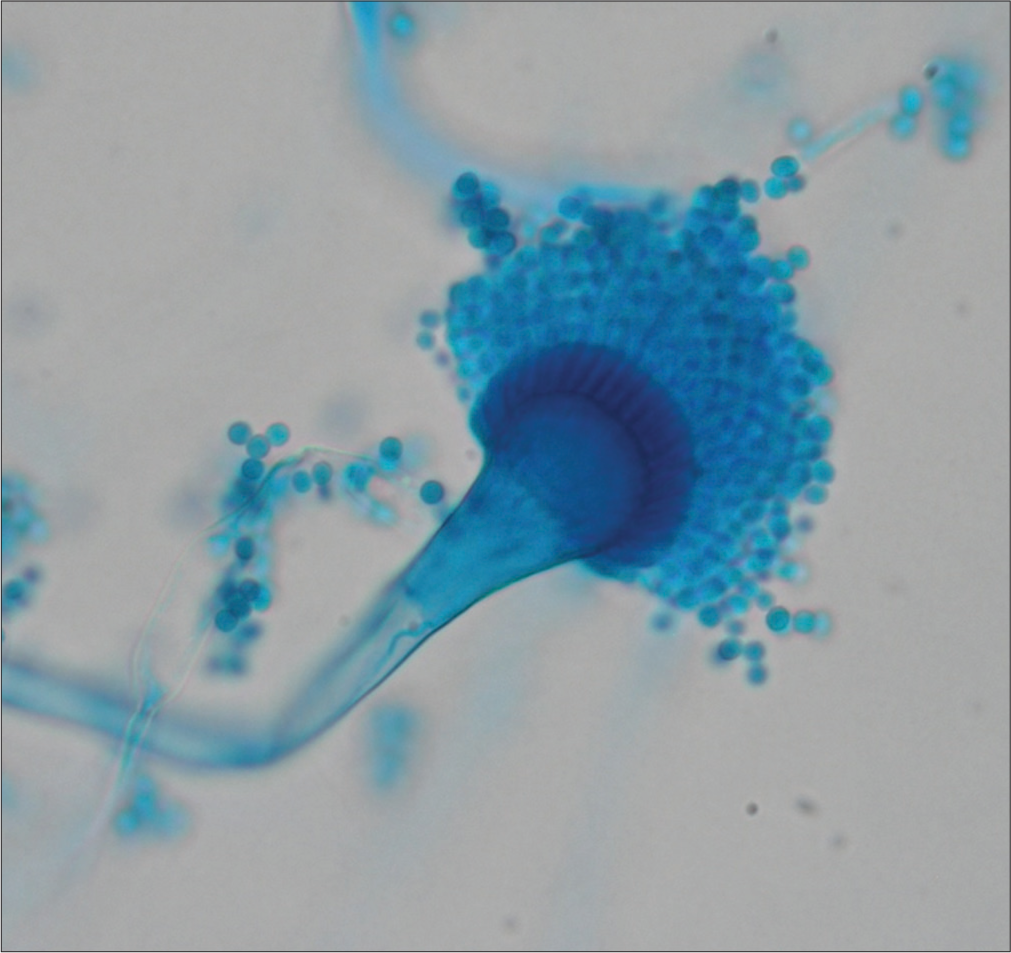
- Direct examination of cultures: Septate, tabulated and hyaline mycelium, as well as Aspergillus heads composed of long conidiophores, round vesicles from which two series of phialides emerge and round microconidia originating from the latter.
DISCUSSION
Notably, in patients with this medical history, contrary to immunocompetent patients, the most frequently isolated microorganism is A. fumigatus, as in this case. Although the exact time of inoculation is unclear, there are well-identified risk factors in this patient, including his occupation in gardening and HIV infection. Although nodular presentation is infrequent, it has been documented, emphasising the importance of considering it in the differential diagnosis. Failure to do so may lead to delayed diagnosis and disease dissemination to other organs, increasing mortality. The treatment of PCA is not entirely clear but includes surgical debridement, antifungal therapy or a combination of both to reduce the risk of recurrence. This patient was treated with surgery and itraconazole for 6 months, and the response was favourable. The literature suggests considering prophylaxis following disease resolution; however, the level of evidence is low, prophylaxis was not administered in this case and the results were great, providing valuable information about the outcome of PCA in an HIV patient with nodular presentation who underwent surgical intervention, oral therapy and no prophylaxis.
CONCLUSION
It is important to consider aspergillosis as a differential diagnosis in patients with solitary nodular lesions, especially in HIV-infected individuals. This case enriches the existing information regarding clinical presentation, response to combination treatment and outcomes in patients with PCA.
Ethical approval
Institutional Review Board approval is not required.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- Primary Cutaneous Aspergillosis in a Patient with CARD9 Deficiency and Aspergillus Susceptibility of Card9 Knockout Mice. J Clin Immunol. 2021;41:427-40.
- [CrossRef] [PubMed] [Google Scholar]
- Primary Cutaneous Aspergillosis Due to Aspergillus fumigatus in an Immunocompetent Patient with Diabetes Mellitus after Tattooing: A Case Report and Review of Literature. Infect Drug Resist. 2023;16:791-7.
- [CrossRef] [PubMed] [Google Scholar]
- Primary Cutaneous Aspergillosis. Acta Derm Venereol. 2010;90:519-20.
- [CrossRef] [PubMed] [Google Scholar]
- Primary Cutaneous Aspergillosis at the Site of Cyanoacrylate Skin Adhesive in a Neonate. Pediatr Dermatol. 2018;35:494-7.
- [CrossRef] [PubMed] [Google Scholar]
- Primary Cutaneous Aspergillosis-An Uncommon Opportunistic Infection Review of the Literature and Case Presentation. J Dtsch Dermatol Ges. 2017;15:839-41.
- [CrossRef] [Google Scholar]








