Translate this page into:
Lupus Miliaris Disseminatus Faciei – A Rare Facial Dermatosis Successfully Treated with Dapsone: A Case Report
*Corresponding author: Subhasree Sarkar, Department of Skin and Venereal Diseases, Indira Gandhi Institute of Medical Sciences, Patna, Bihar, India. subhasreesarkar16@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Sarkar S, Sinha R, Singh A. Lupus Miliaris Disseminatus Faciei – A Rare Facial Dermatosis Successfully Treated with Dapsone: A Case Report. Indian J Postgrad Dermatol. 2024;2:63-5. doi: 10.25259/IJPGD_100_2023
Dear Editor,
A 31-year-old man presented to our outpatient department (OPD) with complaints of multiple asymptomatic brownish lesions over bilateral cheeks, earlobes and forehead for the past 5 months. Initially, the lesions began as few small papules over the left cheek, which then slowly progressed to involve bilateral cheeks, nose, forehead and earlobes. On examination, small (3–5 mm), hyperpigmented, firm, smooth top, monomorphic, brown-coloured papules distributed symmetrically over the cheeks and forehead along with scarring were seen [Figure 1]. There was no history of erythema or flushing due to emotional stresses, food or sun exposure. There was no history of fever or weight loss or any other systemic complaints. There was no history of application of any topical drug and no other body part was affected. Histopathological examination of the biopsy from the left earlobe revealed epithelioid granulomas with areas of necrosis in the mid and deep reticular dermis along with dense periadnexal infiltrate of inflammatory cells composed of lymphocytes, foreign body giant cells, Langhans cells, plasma cells and few neutrophils and eosinophils. Staining with acid–fast bacilli stain and Fite-Faraco stain and tuberculin test was negative. Histopathological impression was consistent with lupus miliaris disseminatus faciei (LMDF) [Figure 2a and b]. His blood counts, erythrocyte sedimentation rate, serum creatinine, liver function tests, fasting blood sugar, serum creatinine, angiotensin-converting enzyme levels and chest X-ray were within normal limits. Based on the clinical and histopathological findings, he was diagnosed with LMDF. The patient was started on oral dapsone (100 mg/day) and the lesions started to regress and healing with scarring was seen [Figure 3]. After 2 months, the dose was tapered to 50 mg/day and stopped after 2 months. No new lesions appeared in the subsequent 1 year of follow-up visits.

- (a) Clinical photograph of the patient at presentation showing hyperpigmented papules and scarring involving the centro-facial area in front profile, (b and c) Right and left profile of the patient respectively.

- (a) Skin biopsy showing stratified squamous epithelial lining. Dermis is infiltrated by granulomas, giant cells, epithelioid cells Hematoxylin & Eosin (×10), lymphocytes, neutrophils, plasma cell and eosinophils. (b) Dermal tissue highlighting granuloma with giant cells and inflammatory cells Hematoxylin & Eosin (×40).
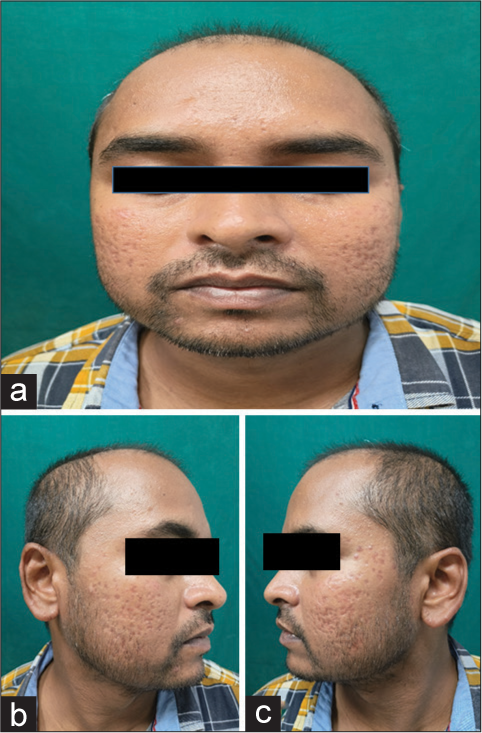
- (a) Clinical photograph of the patient showing complete resolution with scarring after three months in front profile, (b and c) Right and left profile of the patient respectively.
LMDF is an uncommon, idiopathic, chronic granulomatous inflammatory facial dermatosis that was first described by Fox in 1878.[1] It clinically presents as symmetrical, reddish to yellowish-brown or skin-coloured, smooth top, monomorphic papules which have a predilection for the central area of the face characteristically on and around the eyelids, cheeks, forehead, nose, ears, upper lips, chin or neck and affects middle-aged adults.[2] There are some uncommon reports of extra-facial involvements such as the trunk, extremities and genital skin.[3] The papules may occur discreetly or in crops, can be follicular or non-follicular and sometimes have a pustular top. Typically, the lesions last for several months and spontaneous resolution of the lesions, leaving behind small pitted scarring eventually occur after a few years. The name is derived from the historic association with tuberculosis as it was thought to be a form of cutaneous lupus earlier; however, to clear the ambiguity, some authors have advocated using the term facial idiopathic granulomas with regressive evolution (FIGURE) instead of LMDF.[4]
It is postulated that in LMDF, there is an initial role of immune-mediated damage to the hair follicle leading to rupture of the follicle followed by an allergic or foreign body granulomatous response to sebum, keratin or microbial components in the dermis.
The papules of LMDF typically show a yellowish-brown colouration on diascopy which is histologically related to epithelioid cell granulomas. The histological hallmark of LMDF is a granulomatous infiltrate in the dermis which is often centred around pilosebaceous units.
Characteristically, tuberculoid (with central caseation necrosis) granulomas and rarely sarcoidal (non-caseating) has been observed in LMDF. Diffuse infiltrates of inflammatory cells in peri-adnexal pattern without well-formed granulomas may be seen in early lesions and dermal fibrosis is seen in late lesions, which leads to scar formation. The classical features of LMDF on dermoscopy are focal keratotic plugs due to lateral pressure on the hair follicles and correspond histologically to keratin-filled follicular openings.[3,5] Similar granulomatous disorders that might clinically mimic LMDF include granulomatous rosacea, sarcoidosis and infectious diseases such as non-tuberculous mycobacterium infection and deep fungal infections which should be ruled out.
Management of LMDF with systemic tetracycline, low-dose isotretinoin, dapsone, corticosteroids, clofazimine and immunosuppressive drugs has been reported in the literature.[4] Topical therapies, including corticosteroids, calcineurin inhibitors, psoralen combined with ultraviolet-A radiation, 100% trichloroacetic acid as well as carbon dioxide lasers, 1,450 nm diode laser and a non-ablative fractionated 1,565 nm laser may also have a role in the treatment of LMDF. Despite treatment or spontaneous involution, residual pitted scars are a frequent aftermath of LMDF which might lead to cosmetic disfigurement and cause psychological stress to the patients. However, treatment initiation at an early stage may shorten the duration of disease and treatment as well as decrease the tendency and severity of scar formation.
Ethical approval
Institutional Review Board approval is not required.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- Clinical Lecture on Disseminated Follicular Lupus (Simulating Acne) Lancet. 1878;112:75-6.
- [CrossRef] [Google Scholar]
- Lupus Miliaris Disseminatus Faciei. An Bras Dermatol. 2017;92:851-3.
- [CrossRef] [PubMed] [Google Scholar]
- Lupus Miliaris Disseminatus Faciei Part II: An Overview. In: Skinmed. Vol 4. 2005. p. :234-8. Erratum in: Skinmed 2014;12:194. Reddy, Vishwanath [corrected to Belum, Viswanath R]
- [CrossRef] [Google Scholar]
- Nosology and Therapeutic Options for Lupus Miliaris Disseminatus Faciei. J Dermatol. 2011;38:864-73.
- [CrossRef] [PubMed] [Google Scholar]
- Lupus Miliaris Disseminatus Faciei In: StatPearls. Treasure Island, FL: StatPearls Publishing; 2022.
- [Google Scholar]






